
Healthcare Revenue Is Structurally Different
Cash Flow in Healthcare Is Timing-Critical
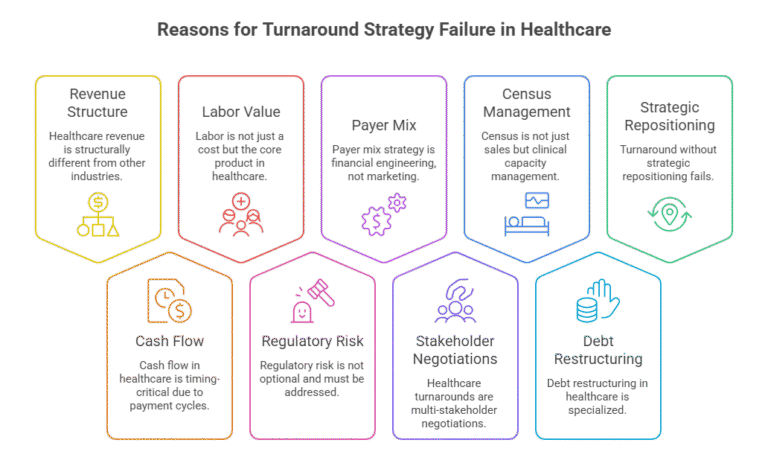
Labor Is Not Just a Cost — It’s the Product
Regulatory Risk Is Not Optional
Payer Mix Strategy Is Not Marketing — It’s Financial Engineering
Healthcare Turnarounds Are Multi-Stakeholder Negotiations
Census Is Not Just Sales — It’s Clinical Capacity Management
Debt Restructuring in Healthcare Is Specialized
Turnaround Without Strategic Repositioning Fails
How Skill Consultants’ Healthcare Expertise Changes the Outcome
Fractional CFO-Level Financial Leadership
Deep Healthcare Financial Modeling
We bring:
1.Fractional CFO-Level Financial Leadership
Strategic liquidity control
Board-ready financial reporting
Covenant monitoring
Cash runway protection
EBITDA stabilization strategies
2. Deep Healthcare Financial Modeling
13-week rolling cash forecasts
Multi-scenario payer modeling
Occupancy sensitivity analysis
Labor cost optimization modeling
Debt restructuring simulations
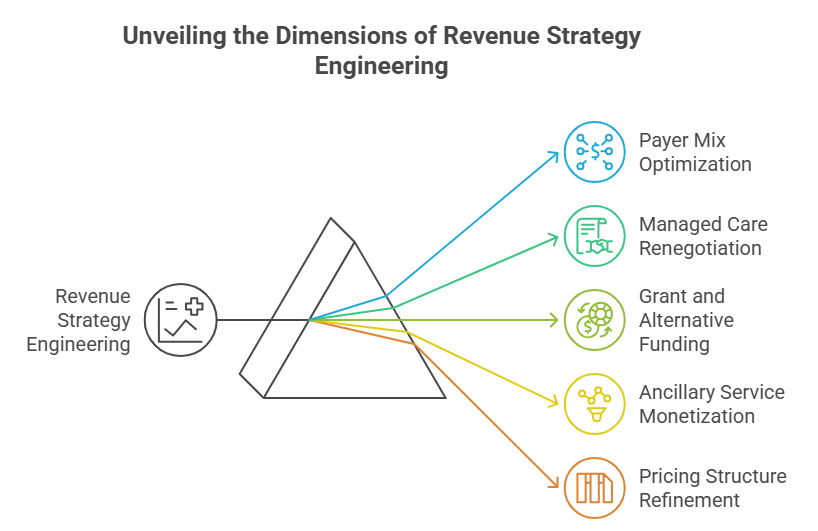
3. Revenue Strategy Engineering
Payer mix optimization
Managed care renegotiation strategy
Grant and alternative funding evaluation
Ancillary service monetization
Pricing structure refinement
4. Operational & Financial Integration
Aligning staffing models with acuity
Reducing agency dependency
Improving revenue cycle efficiency
Controlling expense leakage
5. Data-Driven Decision Frameworks
We turn chaos into structured financial clarity:
Weekly dashboards
Variance tracking
Predictive forecasting
Strategic decision trees
